
Insulin resistance is a metabolic condition in which your cells stop responding properly to insulin, the hormone that moves glucose from the bloodstream into cells for energy. When the cells become resistant, the pancreas produces more insulin to compensate. Blood glucose remains elevated. Fat storage increases. Energy drops.
It is the root driver behind many of the most common health complaints in people over 40: stubborn belly fat, persistent fatigue, brain fog, poor sleep, and relentless sugar cravings.
Most people who have it are never told. This guide explains what insulin resistance is, what causes it, how to identify it in yourself, and exactly how to reverse it.
What Is Insulin Resistance in the Body?
To understand insulin resistance, you need to understand what insulin does in a healthy body.
After you eat, blood glucose rises. The pancreas detects this and releases insulin. Insulin acts like a key, unlocking receptors on your cells so glucose can enter and be used as fuel. Blood sugar drops back to a normal range. The system resets.
In insulin resistance, the lock stops responding to the key. The cells – particularly in muscle, liver, and fat tissue – no longer respond efficiently to the insulin signal. The pancreas compensates by producing more insulin. For a time, blood glucose appears normal. But the underlying dysfunction is worsening with every meal.
Over time, the pancreas cannot keep up. Blood glucose begins to rise. The condition progresses through pre-diabetes and, if unaddressed, into type 2 diabetes.
What Is Insulin Resistance Syndrome?
Insulin resistance is the central feature of a broader condition called metabolic syndrome, also referred to as insulin resistance syndrome.
Metabolic syndrome is diagnosed when a person has three or more of the following markers:
- Elevated waist circumference (above 94cm in men, 80cm in women)
- High triglycerides (above 1.7 mmol/L)
- Low HDL cholesterol
- Elevated blood pressure (above 130/85 mmHg)
- Elevated fasting glucose (above 5.6 mmol/L)
Each of these conditions links back to insulin dysregulation. Treating them individually without addressing the underlying insulin resistance produces limited results. Addressing insulin resistance directly tends to improve all of them simultaneously.
What Causes Insulin Resistance?
Insulin resistance develops as a result of several overlapping factors, most of which are diet and lifestyle-driven.
Diet: Chronic consumption of refined carbohydrates and sugar keeps insulin persistently elevated. Cells exposed to high insulin over time progressively downregulate their response. This is the most direct dietary cause.
Physical inactivity: Skeletal muscle is the body’s primary site for glucose disposal. When muscle is not being used, glucose uptake decreases, and insulin has to work harder to maintain normal blood sugar levels.
Excess visceral fat: Fat stored around the abdominal organs – as distinct from subcutaneous fat under the skin – releases inflammatory molecules that directly impair insulin signalling at the cellular level.
Poor sleep: A single night of poor sleep measurably reduces insulin sensitivity the following day. Chronic sleep deprivation is a consistent and under-recognised driver of metabolic dysfunction.
Chronic stress: Cortisol raises blood glucose as part of the body’s stress response. Persistently elevated cortisol means persistently elevated insulin – even in the absence of food.
Age: Insulin sensitivity naturally declines after 40. This makes the 40-60 age group particularly vulnerable – and makes early intervention particularly worthwhile.
Genetic predisposition: Family history of type 2 diabetes or metabolic syndrome increases risk. Genetics loads the gun; lifestyle pulls the trigger.
What Are the Symptoms of Insulin Resistance?
Insulin resistance does not cause dramatic symptoms. It causes a background noise of complaints that are easy to dismiss as stress, ageing, or poor sleep. This is why it goes unidentified for so long.
The most common symptoms:
- Energy crashes after meals, particularly after carbohydrate-heavy ones
- Persistent fatigue that is not resolved by sleep
- Strong cravings for sugar or refined carbohydrates, especially in the afternoon
- Belly fat that accumulates around the abdomen and resists conventional dieting
- Brain fog and difficulty concentrating, often worse after eating
- Poor sleep quality despite feeling tired
- Slow or stalled weight loss despite eating less
- Skin tags around the neck, armpits, or groin (a documented marker)
- Increased thirst or frequent urination in more advanced cases
If several of these are present simultaneously, insulin resistance is a likely underlying cause.
Insulin resistance symptoms in females
Women may experience additional symptoms related to hormonal disruption caused by elevated insulin. Polycystic ovary syndrome (PCOS) is directly linked to insulin resistance in a significant proportion of cases. Irregular periods, acne, and excess facial or body hair can all indicate elevated insulin, which drives hormonal imbalance. Insulin resistance also worsens perimenopausal symptoms in women over 40.
Insulin resistance symptoms in males
Men tend to accumulate visceral fat more readily than women, making abdominal weight gain a particularly prominent early sign. Elevated insulin also suppresses testosterone production, which can contribute to low libido, reduced muscle mass, and fatigue, often attributed to “low T” rather than the metabolic condition driving it.
How to Tell If You Have Insulin Resistance?
Insulin resistance is not routinely tested for on standard blood panels, which is a significant gap in conventional healthcare. A normal fasting glucose result does not rule it out – insulin resistance can be established for years before glucose rises to flagged levels.
The most revealing tests:
Fasting insulin:
A fasting insulin level above 10 mU/L is a strong indicator of insulin resistance, even when glucose appears normal. This test is not usually ordered unless specifically requested.
HOMA-IR:
Calculated from fasting glucose and fasting insulin. A score above 2.0 suggests developing resistance; above 2.9 is significant. Your GP can calculate this from standard lab values if you request both figures.
HbA1c:
A three-month average of blood glucose. Useful, but a later-stage indicator.
Triglyceride-to-HDL ratio:
A ratio above 2.0 mmol/L is one of the strongest indirect markers of insulin resistance available on a standard lipid panel.
If you suspect insulin resistance, specifically request a fasting insulin test. Most GPs will not order it without prompting.
What Is Insulin Resistance in Type 2 Diabetes?
Type 2 diabetes does not appear suddenly. It is the endpoint of a progression that typically begins with insulin resistance years – often a decade or more – earlier.
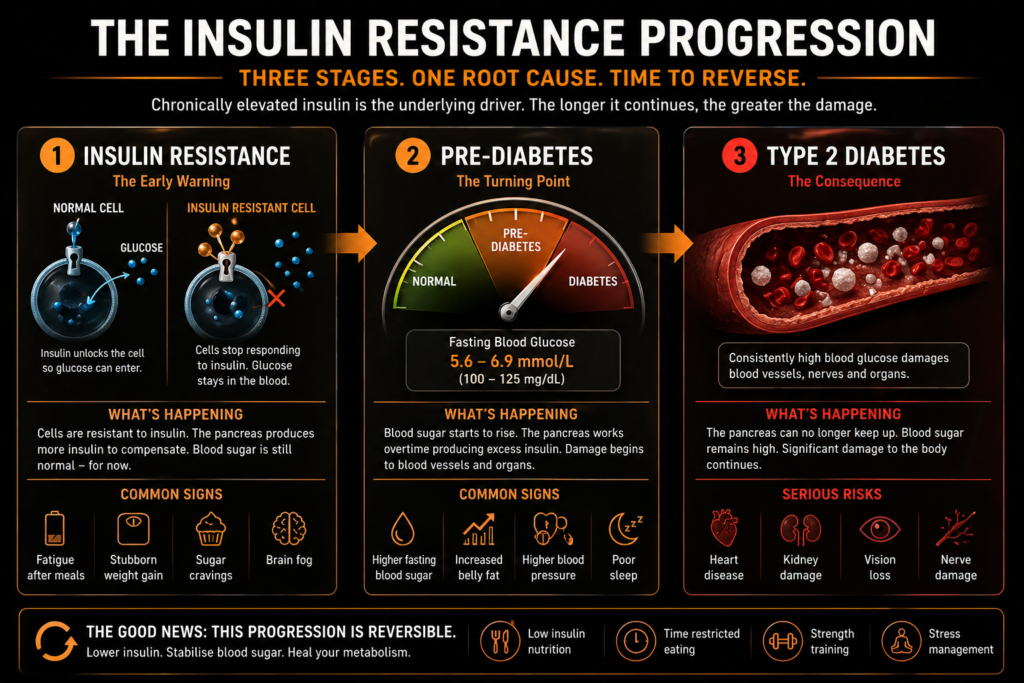
The stages:
Type 2 diabetes: The pancreas can no longer maintain normal glucose levels. Fasting glucose exceeds 7.0 mmol/L, or HbA1c exceeds 48 mmol/mol.
Insulin resistance: Cells become less responsive. The pancreas compensates with more insulin. Blood glucose may appear normal.
Pre-diabetes: Compensation begins to fail. Fasting glucose rises above 5.5 mmol/L. HbA1c reaches 42-47 mmol/mol. This is the critical intervention window.
The important point is that the earlier the intervention, the more reversible the condition. Pre-diabetes is largely reversible. Even established type 2 diabetes can be put into remission through sustained dietary change. Insulin resistance, caught early, is highly responsive to the right approach.
Is Insulin Resistance Curable?
Yes – with an important clarification on terminology.
“Curable” implies a permanent fix that requires no ongoing maintenance. Insulin resistance is not curable in that sense. It is, however, fully reversible – meaning that with the right dietary and lifestyle changes, insulin sensitivity can be restored to normal levels, symptoms resolve, and the metabolic risks associated with the condition are eliminated.
The distinction matters because the same factors that drove insulin resistance – excess refined carbohydrates, inactivity, poor sleep, chronic stress – will drive it back if reintroduced. Reversal is real; maintenance is required.
What’s the fastest way to cure insulin resistance?
The fastest improvements come from a combination of: significantly reducing dietary carbohydrate, introducing a structured eating window (intermittent fasting), walking after meals, and prioritising sleep. This combination can produce measurable improvements in fasting insulin within days, and meaningful changes in HOMA-IR within two to four weeks.
Yes, it’s Reversible! Here’s Where to Start: Get The 3-Day Protocol
Insulin Resistance Treatment – The Evidence-Based Approach
The most effective interventions for insulin resistance are dietary and lifestyle-based. No medication reverses insulin resistance – medication manages its consequences.
1. Low-carbohydrate diet:
Reducing carbohydrate intake is the most direct way to lower the insulin demand in the body. A low-carbohydrate or ketogenic diet has been shown to improve insulin sensitivity rapidly – often within the first week.
2. Intermittent fasting:
Extended periods without food allow insulin levels to fall. Sustained periods of low insulin restore cellular receptor sensitivity over time. A 16:8 eating window is the most accessible starting point.
3. Post-meal movement:
A 10-15 minute walk after eating reduces the post-meal glucose spike by up to 30%. This is one of the highest-leverage habits available.
4. Resistance training:
Building muscle mass increases the body’s capacity to dispose of glucose without insulin. Even two sessions per week produce measurable improvements in insulin sensitivity.
5. Sleep optimisation:
Seven to nine hours of quality sleep per night is not optional for metabolic recovery. Sleep deprivation directly impairs insulin signalling regardless of diet.
6. Stress reduction:
Lowering chronic cortisol reduces the background insulin elevation that stress creates. The mechanism is real, and the effect is significant.
The 5 Key Indicators of Insulin Resistance
For a quick self-assessment, these are the five most reliable indicators:
- Fasting insulin above 10 mU/L on a blood test
- Waist circumference above 94cm (men) or 80cm (women)
- Triglyceride-to-HDL ratio above 2.0
- Energy crash within 90 minutes of eating carbohydrates
- Belly fat that does not respond to conventional caloric restriction
If three or more apply, insulin resistance is likely present and worth addressing.
Start Here: The 3-Day Metabolic Reset
The fastest way to begin reversing insulin resistance is to remove the biggest insulin drivers – refined carbohydrates, sugar, frequent snacking – and introduce a structured eating window. The first 72 hours are when the most significant metabolic shift occurs.
The free 3-Day Metabolic Reset gives you the exact protocol: what to eat, when to eat, and what to expect as your metabolism begins to reset.
